nursing head to toe assessment pdf
A head-to-toe nursing assessment is a comprehensive process that reviews the health of major body systems. Nurses commonly perform this as part of a physical exam, ensuring a thorough evaluation of a patient’s condition.
Definition and Purpose of Head-to-Toe Assessment
A head-to-toe assessment is a systematic and comprehensive physical examination used to collect patient data and determine their health status. It involves examining the entire body, from head to toe, in a thorough manner. The primary purpose is to identify any health issues, providing a clear understanding of the patient’s overall physical condition. This assessment helps healthcare providers gather crucial information for formulating an effective treatment plan and addressing any potential concerns. It’s a vital part of the nursing process, ensuring that no aspect of the patient’s health is overlooked. This comprehensive approach aids in early detection and intervention, promoting optimal patient outcomes.

Essential Components of a Head-to-Toe Assessment
A successful head-to-toe assessment requires proper equipment and a systematic approach. Documentation of findings is also crucial for effective patient care and follow-up.
Gathering Necessary Equipment
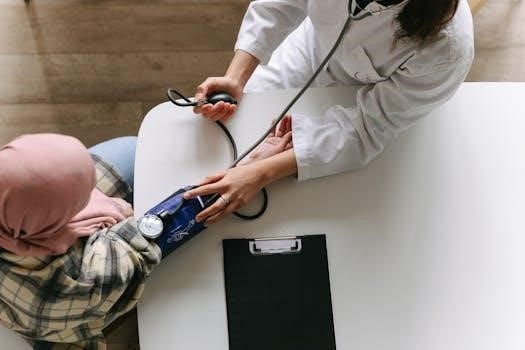
Before initiating a head-to-toe assessment, collecting all essential equipment is paramount for an efficient and thorough examination. This includes a stethoscope for auscultation, a thermometer to measure body temperature, and a blood pressure cuff of appropriate size. A pulse oximeter is needed to assess oxygen saturation, and a scale and tape measure for anthropometric data. Additionally, a penlight is crucial for eye and oral assessments, and a reflex hammer is useful for neurological checks. Finally, have documentation equipment readily available for accurate recording of findings. Having these items prepared ensures a smooth assessment process.
Systematic Approach and Documentation
A systematic approach is vital for conducting a thorough head-to-toe assessment. This ensures no body system is overlooked, and findings are accurately recorded. Nurses should follow a logical sequence, moving from head to toe, to maintain consistency. Proper documentation is equally important. All findings, both normal and abnormal, must be clearly and concisely written down. This documentation serves as a crucial reference for future care and allows for comparison over time. Students should integrate these components in their assessments, adapting techniques to the patient’s age and specific needs. This meticulous process ensures quality patient care.
Key Assessment Techniques
Key assessment techniques include inspection, palpation, percussion, and auscultation. These methods help nurses gather objective data about a patient’s physical condition during the head-to-toe assessment.
Inspection, Palpation, Percussion, Auscultation
These four techniques form the foundation of a comprehensive physical assessment. Inspection involves visual observation of the patient’s body, noting any abnormalities. Palpation uses touch to assess texture, temperature, and masses. Percussion uses tapping to assess underlying tissue density. Auscultation utilizes a stethoscope to listen to body sounds, such as heart and lung sounds. These methods provide valuable data for understanding a patient’s overall health status. Mastering these techniques is crucial for accurate and effective nursing assessments, aiding in the identification of potential health issues and the formulation of appropriate care plans. Each technique offers unique insights, and their combined use ensures a thorough evaluation.
Specific Body Systems Assessment
This section delves into the detailed assessment of individual body systems. It covers vital areas like the cardiovascular, respiratory, neurological, and musculoskeletal systems, providing a comprehensive health evaluation.
General Survey and Vital Signs
The general survey is the initial step in a head-to-toe assessment, providing clues about the client’s overall health. This includes observing the patient’s general appearance and mental status. The chief complaint, or main reason for seeking care, is identified. Vital signs such as temperature, pulse, respiration rate, and blood pressure are measured. These objective data points establish a baseline for further assessment and inform the health care professional on the patients overall condition. Any unusual findings should be followed up with a focused assessment specific to the affected body system.
Skin, Hair, and Nails Assessment
The skin, hair, and nails are external structures that provide valuable insights into a patient’s health. A thorough assessment involves inspecting and palpating these areas, noting any abnormalities. This includes assessing skin color, temperature, moisture, and texture. Hair distribution, texture, and scalp condition are also evaluated. Nail shape, color, and thickness are examined to identify potential issues. Changes in these structures may indicate local or systemic problems. The nurse needs to collect data about current symptoms, the clients past and family history, and lifestyle and health practices.
Head and Neck Assessment
The head and neck assessment focuses on several key areas, including the cranium, face, thyroid gland, and lymph nodes. During this assessment, the nurse inspects the head for size, shape, and any visible abnormalities. The face is examined for symmetry, skin condition, and facial expressions. Palpation of the thyroid gland helps to identify any enlargement or tenderness. The lymph nodes in the head and neck region are also palpated to check for swelling or tenderness, which may indicate infection or other health issues. Gathering data in this area provides important information about the patient’s overall health.
Eye and Vision Assessment
A thorough eye and vision assessment requires a good understanding of the external and internal structures of the eye, visual fields, pathways, and reflexes. The nurse should inspect the external eye structures for any abnormalities, such as redness, swelling, or lesions. Visual acuity is also assessed to determine the patient’s ability to see clearly at different distances. The nurse will also evaluate the pupils for size, shape, and reactivity to light. Any reported symptoms or signs need to be investigated further, including family history, as this can provide crucial data for understanding the patient’s overall condition related to their vision.
Ear and Hearing Assessment
The assessment of hearing begins when the nurse first interacts with the client, providing crucial insights into the client’s ability to engage with their environment. Subjective data gathered during the assessment includes any difficulties the patient reports related to hearing, such as tinnitus or vertigo. The nurse will also inspect the external ear for abnormalities. Further tests may be necessary to determine the extent of any hearing loss or issues with balance. Gathering information about family history is also important for a comprehensive ear and hearing assessment. It is essential to understand the client’s hearing ability to provide appropriate care and communication strategies.
Mouth, Throat, Nose, and Sinus Assessment
Subjective data concerning the mouth, throat, nose, and sinuses aids in identifying diseases and abnormalities which could affect a client’s daily activities. The nurse should inquire about symptoms like sore throat, difficulty swallowing, nasal congestion, or sinus pain. Additionally, a thorough examination involves inspecting the oral mucosa, teeth, and gums, as well as assessing the condition of the nose and sinuses. Any reported symptoms should be further explored to understand their impact on the client’s health and well-being. This holistic approach ensures that all contributing factors are considered and addressed appropriately.
Thoracic and Lung Assessment
Subjective data from the thoracic and lung assessment provides critical clues about potential respiratory problems and guides nursing diagnoses. This includes gathering information about symptoms like cough, shortness of breath, chest pain, and any history of respiratory illnesses. The nurse should also explore factors that may increase the client’s risk for lung disorders. Additionally, the assessment involves a thorough physical examination, including inspection of the chest wall, palpation for tenderness or masses, and auscultation to assess breath sounds. These combined findings help determine the client’s respiratory status and inform appropriate interventions and care planning.
Breast Assessment (Non-Pregnant Women)
This section focuses on the examination of the breasts in non-pregnant women. It’s crucial to remember that if a client reports any symptoms, a thorough symptom analysis must be performed. This includes evaluating the characteristics of any lumps, pain, or nipple discharge, as well as exploring associated factors. The assessment should also involve palpation of the breast tissue, including the axillary lymph nodes, to identify any abnormalities. The nurse must be sensitive to the client’s feelings and concerns during this assessment, while ensuring a comprehensive evaluation.
Heart and Neck Vessels Assessment
Subjective data collected about the heart and neck vessels helps the nurse identify abnormal conditions potentially impacting a client’s ability to perform daily activities and fulfill responsibilities. It is crucial for the nurse to inquire about seemingly minor symptoms, as well as personal and family history of vascular disease. Evaluating lifestyle and health factors that may impair cardiovascular health is also essential. The assessment includes inspection, palpation, and auscultation of the heart and neck vessels, focusing on any irregularities or deviations from normal findings and any associated symptoms.
Peripheral Vascular Assessment
In a peripheral vascular assessment, nurses gather crucial data by asking patients about symptoms they might consider unimportant. A thorough evaluation includes personal and family history of vascular disease. It is essential to evaluate aspects of the client’s lifestyle and health factors which can impair peripheral vascular health. The assessment focuses on inspecting and palpating peripheral pulses, assessing skin color, temperature, and capillary refill. It also includes evaluating for edema, varicosities, and any other signs of peripheral vascular disease which could contribute to health issues and impact daily function.
Abdominal Assessment
The abdominal assessment involves collecting subjective data about symptoms of specific abdominal organs. This includes the function of the digestive system, nutritional habits, and usual bowel patterns. Always follow the sequence of inspection, auscultation, percussion, and palpation, as altering this order may affect bowel sound frequency. Data focus on identifying any digestive issues, discomfort, and changes in elimination patterns. It provides a comprehensive understanding of the client’s abdominal health, which can help guide treatment plans and identify potential problems. This data is critical for assessing the digestive system’s overall condition and any related issues.
Reproductive System and Genitalia Assessment
When discussing the reproductive system and genitalia, be mindful of sensitivities surrounding body image, sexuality, and fears of cancer. Consider the client’s cultural background when interviewing. In some cases, your gender may impact the accuracy of the findings. This is a sensitive topic for both client and examiner. The assessment involves gathering subjective data to identify potential health risks and concerns. The goal is to provide culturally sensitive and respectful care while obtaining the necessary information for accurate evaluation. It requires a delicate approach to ensure comfort and openness.

Musculoskeletal Assessment
The musculoskeletal assessment evaluates the client’s ability to perform daily activities and assesses their level of functioning. This system’s evaluation helps in identifying limitations and areas of concern that may affect mobility and independence. It involves assessing the bones, muscles, joints, and associated structures. The process includes observing range of motion, muscle strength, and any deformities or abnormalities. It is essential to gather subjective data regarding pain, stiffness, or difficulty moving. This assessment plays a vital role in formulating a comprehensive plan of care by identifying physical limitations. It is also crucial to monitor progression of any conditions.
Neurological Assessment
The neurological assessment is crucial because problems within this system can influence other body functions and vice-versa; This evaluation includes assessing the patient’s mental status, cranial nerves, motor function, sensory function, and reflexes. It helps identify any abnormalities or changes in neurological status. The assessment often includes evaluating the patient’s level of consciousness, orientation, and cognitive abilities. It’s essential to note any deficits or changes in motor skills, such as weakness or paralysis. Sensory function is tested to identify numbness or tingling. Reflexes are checked to determine the integrity of the nervous system. The nurse carefully documents all findings to monitor neurological changes.

